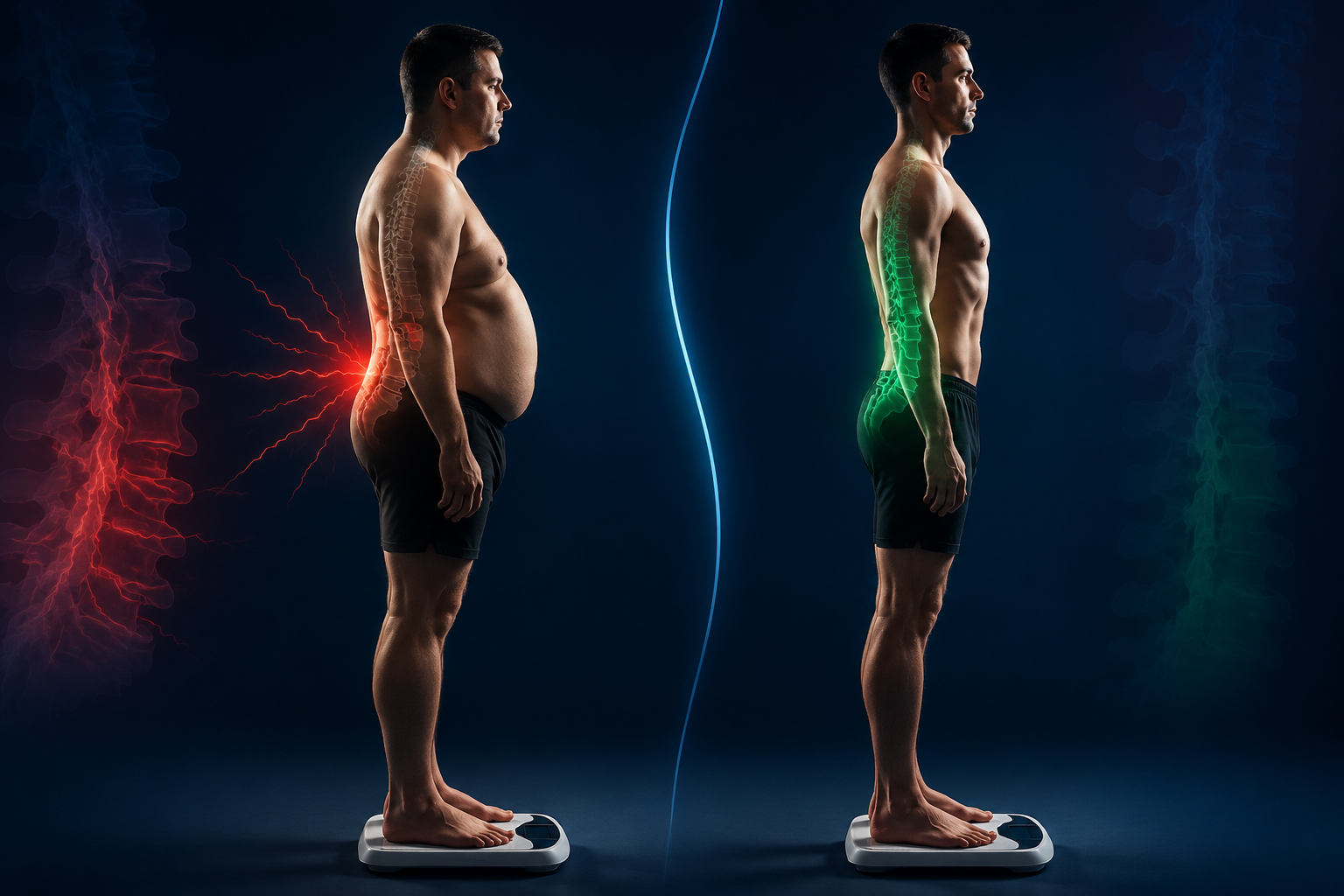
Yes, losing weight helps back pain significantly. Every pound lost removes up to four pounds of pressure from your lower back, reducing stress on spinal discs and joints. Studies show that people who lose just 5% of their body weight experience measurable pain relief and improved mobility, with greater weight loss producing even stronger results.
Key Takeaways
Weight loss reduces mechanical load: Each pound lost decreases spinal pressure by up to 4 pounds, relieving compressed discs and joints
5% weight loss threshold: Losing 5% of body weight produces clinically significant pain relief in most chronic back pain sufferers
Multiple relief mechanisms: Weight loss reduces inflammation, improves circulation, strengthens core stability, and enhances posture
BMI correlation: Each BMI unit increase (roughly 10 pounds) raises back pain risk by 7% in large population studies
Sustainable approach works best: Gradual weight loss through diet and exercise produces lasting relief compared to rapid methods
Combined strategies amplify results: Weight loss paired with inversion therapy and core strengthening delivers superior outcomes
Timeline matters: Most people notice initial improvements within 8-14 weeks of consistent weight loss efforts
Not a complete cure: Weight loss significantly reduces pain but works best as part of comprehensive back pain treatment
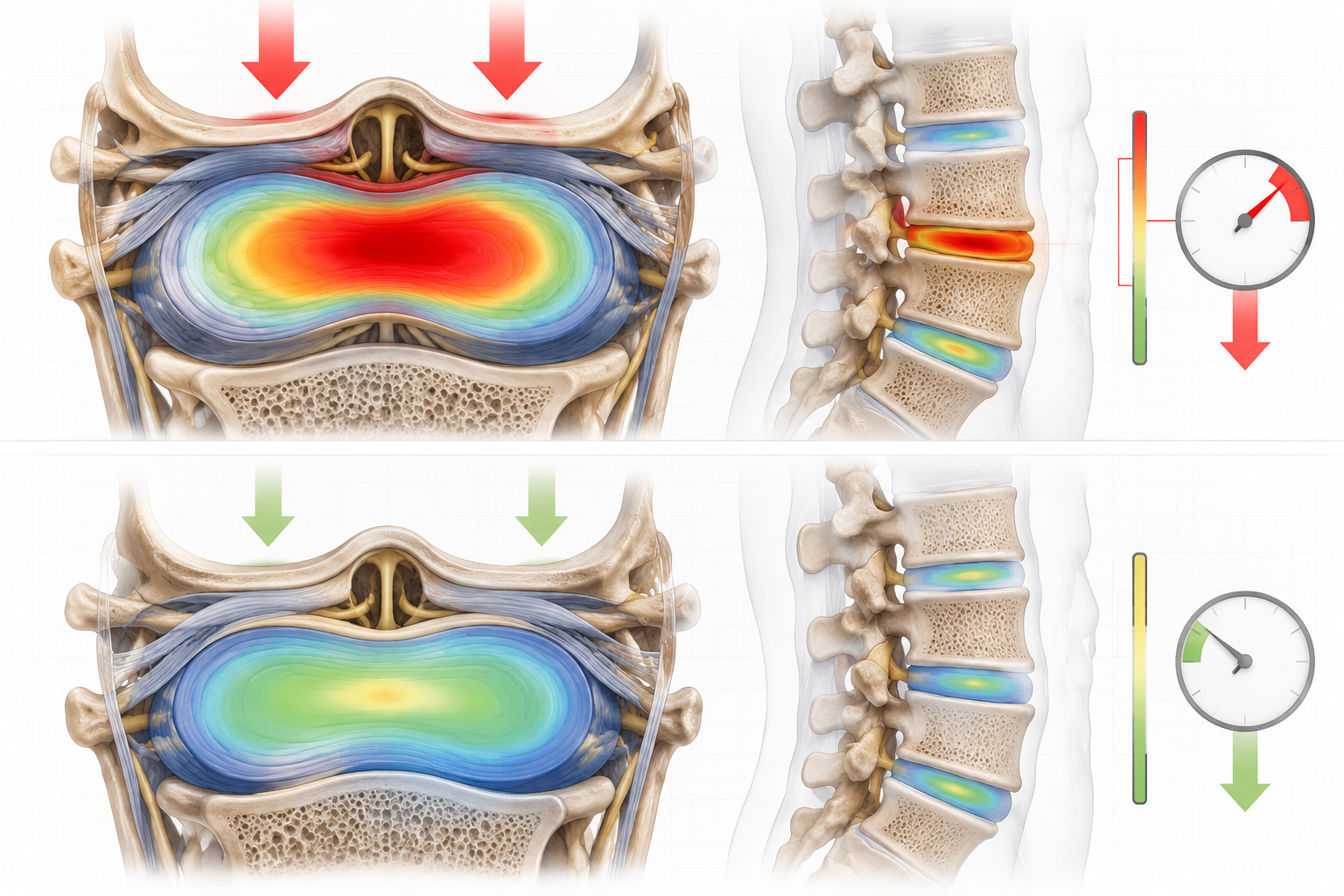
How Does Excess Weight Cause Back Pain?
Excess weight creates back pain through direct mechanical stress on your spine. Your lower back bears the burden of supporting your upper body weight, and every additional pound multiplies that load. Think of your spine as a suspension bridge: adding weight beyond its design capacity strains the cables and support structures until something gives.
The lumbar region absorbs the greatest impact because it sits at the body’s center of gravity. When you carry excess weight, especially around your midsection, your center of gravity shifts forward. This forces your spine into unnatural positions to maintain balance.
Primary mechanisms of weight-related back pain:
Disc compression: Extra weight squeezes intervertebral discs, reducing their shock-absorbing capacity and accelerating degeneration
Joint overload: Facet joints experience excessive friction and wear, triggering inflammation and pain
Postural distortion: Anterior pelvic tilt and excessive lumbar curve develop to compensate for abdominal weight
Muscle imbalance: Core muscles weaken while back muscles overwork, creating chronic tension and fatigue
Ligament strain: Spinal ligaments stretch beyond normal range, losing their supportive function
Large-scale research involving over 110,000 patients demonstrates that back pain prevalence increases 7% for each BMI unit gained between 18 and 35. This linear relationship confirms that weight directly influences spinal health, making weight management a critical factor in spine health maintenance.
Does Losing Weight Help Back Pain Relief?
Losing weight provides substantial back pain relief through multiple biological pathways. A 2024 study found that even modest weight loss reduced pain prevalence, severity, and intensity in chronic musculoskeletal pain patients, with improvements occurring regardless of baseline pain levels.
The relief mechanism operates on a simple principle: reducing load decreases stress. When you lose weight, you immediately decrease the compressive forces acting on your spinal structures. This allows discs to rehydrate, joints to recover, and inflammation to subside.
Evidence-based outcomes from weight loss studies:
Weight Loss AmountPain Relief ResultStudy Population>5% body weight50% achieved clinically significant pain reduction46 obese adults, 14 weeks>5% body weightSignificant low back pain reductionEuropean Journal of Pain, 201910 pounds (200 lb person)Removes 40 pounds of spinal pressureBiomechanical analysisVariable BMI reduction73% showed improved disability scoresCanadian pilot study
A Canadian pilot study of 46 obese adults with mild-to-severe back pain revealed impressive results: 98% lost more than 5% of their body weight after 14 weeks in a supervised program. Among these participants, 50% reported clinically significant pain relief, and 73% showed improved disability scores.
Choose weight loss as your primary intervention if you have a BMI over 25 and chronic back pain without acute injury. The approach works best for mechanical back pain rather than pain from specific injuries or structural abnormalities. Combine weight loss with back pain relief strategies for optimal results.
What Are the Biological Mechanisms Behind Weight Loss and Pain Relief?
Weight loss triggers multiple biological mechanisms that collectively reduce back pain. These mechanisms operate simultaneously, creating a compounding effect that exceeds simple load reduction.
Biomechanical mechanisms:
Pressure reduction: Every pound lost removes up to 4 pounds of force from lumbar discs and facet joints
Improved disc function: Reduced compression allows discs to rehydrate and regain height, restoring cushioning capacity
Postural restoration: Natural spinal curves return as anterior pelvic tilt decreases and core stability improves
Enhanced mobility: Reduced load enables greater range of motion without pain, creating a positive feedback loop
Immunoendocrine mechanisms:
Decreased inflammation: Adipose tissue produces inflammatory cytokines; less fat means fewer inflammatory molecules circulating through your body
Improved circulation: Better blood flow delivers oxygen and nutrients to spinal structures, accelerating healing
Hormonal balance: Weight loss normalizes hormones that influence pain perception and tissue repair
Reduced oxidative stress: Lower body fat decreases cellular damage that contributes to chronic pain
Psychosocial mechanisms:
Improved mental health: Weight loss success boosts mood and reduces depression, which amplifies pain perception
Enhanced self-efficacy: Achieving weight loss goals increases confidence in managing pain through lifestyle changes
Better sleep quality: Reduced weight often improves sleep, which is critical for pain management and tissue recovery
Increased activity tolerance: As pain decreases, you can exercise more, which further supports weight loss and pain relief
These mechanisms work together synergistically. The inflammatory reduction from fat loss enhances the benefits of decreased mechanical load, while improved mental health increases your capacity to maintain healthy behaviors. This creates a virtuous cycle where each improvement reinforces the others.
For people with sciatica treatment needs, weight loss specifically reduces pressure on nerve roots, decreasing radiating leg pain alongside back discomfort.
How Much Weight Loss Is Needed for Back Pain Relief?
The threshold for meaningful back pain relief starts at 5% of your total body weight. This represents 10 pounds for a 200-pound person or 12.5 pounds for someone weighing 250 pounds. Research consistently identifies this 5% threshold as the point where clinically significant improvements begin.
Weight loss targets and expected outcomes:
5% body weight loss: Initial pain reduction, improved mobility, decreased inflammation markers
10% body weight loss: Substantial pain relief, significant disability improvement, enhanced quality of life
15% body weight loss: Major pain reduction, potential elimination of chronic pain in some cases, dramatic functional improvements
A 2019 European study observed that patients losing more than 5% of their body weight experienced significant low back pain reductions, with greater weight loss producing proportionally better results. The relationship between weight loss and pain relief appears dose-dependent: more weight lost generally equals more pain relief.
However, the relationship isn’t perfectly linear. Some people experience dramatic relief with modest weight loss, while others require more substantial changes. Individual factors influence outcomes:
Pain duration: Chronic pain of longer duration may require more weight loss for equivalent relief
Structural damage: Existing disc degeneration or arthritis may limit improvement potential
Body composition: Losing visceral (abdominal) fat produces better results than subcutaneous fat loss
Activity level: Combining weight loss with exercise amplifies benefits beyond weight loss alone
Set realistic expectations: aim for 5-10% weight loss over 3-6 months as an initial goal. This pace allows sustainable habit changes while producing measurable pain relief. Avoid crash diets or extreme approaches, which often lead to muscle loss and can actually worsen back pain.
For those exploring complementary approaches, benefits of inversion therapy for lasting back relief can enhance weight loss efforts by reducing pain during exercise and improving spinal health.
What Is the Timeline for Seeing Back Pain Improvement from Weight Loss?
Most people notice initial back pain improvements within 8-14 weeks of consistent weight loss efforts. This timeline aligns with the period required to lose 5% of body weight at a healthy pace of 1-2 pounds per week.
Expected timeline for pain relief:
Weeks 1-4: Minimal pain change; focus on establishing sustainable habits and initial weight loss
Weeks 5-8: First noticeable improvements in mobility and reduced pain during specific activities
Weeks 9-14: Clinically significant pain reduction for many people; improved disability scores
Weeks 15-26: Continued improvement with sustained weight loss; enhanced quality of life and function
Beyond 6 months: Maintenance phase; pain relief stabilizes at new baseline with continued healthy weight
The Canadian pilot study that achieved 98% success in weight loss showed measurable pain improvements at the 14-week mark, with 50% of participants reaching clinically significant pain relief thresholds. This suggests that three to four months represents a critical milestone for most people.
Individual variation affects this timeline significantly. Factors that accelerate pain relief include:
Starting with higher BMI (more weight to lose produces faster initial results)
Combining weight loss with physical therapy or spinal decompression techniques
Focusing on anti-inflammatory nutrition alongside calorie reduction
Incorporating core strengthening exercises as pain allows
Maintaining consistent sleep and stress management practices
Factors that may delay pain relief include:
Severe structural damage requiring more extensive weight loss
Continued inflammatory diet despite calorie reduction
Sedentary lifestyle without movement therapy
Poor sleep quality interfering with tissue recovery
Underlying medical conditions affecting healing capacity
Track your progress using both objective measures (weight, BMI, waist circumference) and subjective assessments (pain scales, disability questionnaires, activity tolerance). This dual approach helps you identify improvements even when pain relief feels gradual.
What Weight Loss Methods Work Best for Back Pain Relief?
The most effective weight loss methods for back pain relief combine calorie reduction with anti-inflammatory nutrition and appropriate physical activity. Supervised programs that address multiple factors simultaneously produce superior results compared to single-intervention approaches.
Evidence-based weight loss strategies:
Dietary approaches:
Calorie deficit: Create a 500-750 calorie daily deficit for 1-2 pounds weekly loss
Anti-inflammatory foods: Emphasize omega-3 fatty acids, colorful vegetables, berries, and whole grains
Protein prioritization: Maintain 0.8-1.0 grams per pound of target body weight to preserve muscle mass
Processed food reduction: Minimize refined sugars, trans fats, and inflammatory seed oils
Hydration focus: Adequate water intake supports disc hydration and metabolic function
Physical activity modifications:
Low-impact cardio: Walking, swimming, cycling, or elliptical training that doesn’t aggravate pain
Progressive core strengthening: Gentle exercises that build spinal support without excessive load
Flexibility work: Stretching and mobility exercises that improve range of motion
Activity pacing: Gradual increase in duration and intensity as pain allows
Movement variety: Multiple short activity sessions rather than single prolonged efforts
Behavioral and support elements:
Professional supervision: Working with healthcare providers, dietitians, or physical therapists
Accountability systems: Regular weigh-ins, food logging, or support group participation
Stress management: Meditation, breathing exercises, or counseling to address emotional eating
Sleep optimization: Consistent sleep schedule and sleep hygiene practices
Environmental modification: Removing temptations and creating supportive home environments
The Canadian pilot study that achieved exceptional results used a supervised multidisciplinary program combining dietary counseling, exercise prescription, and behavioral support. This comprehensive approach addresses the complex relationship between weight, pain, and lifestyle factors.
Avoid extreme approaches that promise rapid results. Very low-calorie diets, excessive exercise while in pain, or surgical interventions should be reserved for specific cases under medical supervision. These methods can worsen back pain through muscle loss, injury risk, or metabolic complications.
Consider how food choices boost your inversion table results when combining weight loss with complementary therapies. Nutrition affects both weight management and spinal health through multiple pathways.
Can Weight Loss Alone Eliminate Back Pain?
Weight loss alone eliminates back pain for some people but not everyone. The outcome depends on the underlying cause of your pain, the extent of structural damage, and individual factors affecting healing capacity.
When weight loss alone may eliminate pain:
Mechanical back pain caused primarily by excess load without structural damage
Recent-onset pain (less than 6 months) without chronic changes
Younger individuals with better healing capacity and minimal degeneration
Pain that improves significantly with rest and worsens with activity
No neurological symptoms or radiating pain patterns
When weight loss needs complementary treatments:
Chronic pain lasting more than 12 months with established pain patterns
Structural issues like herniated discs, spinal stenosis, or significant arthritis
Neurological symptoms including numbness, tingling, or weakness
Pain that persists regardless of position or activity level
Multiple contributing factors beyond weight (poor posture, weak core, stress)
Research shows that weight loss produces the best outcomes when combined with other interventions. A comprehensive approach addresses multiple pain contributors simultaneously, creating synergistic effects that exceed any single treatment.
Effective complementary treatments to combine with weight loss:
Physical therapy: Targeted exercises that strengthen supporting muscles and improve movement patterns
Inversion therapy: Spinal decompression that reduces disc pressure and improves circulation
Manual therapy: Chiropractic care or massage that addresses soft tissue restrictions and joint dysfunction
Pain education: Understanding pain mechanisms that reduces fear-avoidance and improves coping
Ergonomic modifications: Workplace and home adjustments that reduce daily spinal stress
Post-bariatric surgery data reveals mixed results regarding pain elimination. While some studies show moderate correlation between BMI reduction and pain improvement, others find no significant relationship. One study documented 51% reduction in low back pain prevalence at 22.5 months post-surgery, but this still left nearly half of patients with ongoing pain.
This evidence suggests that weight loss provides substantial benefit but rarely serves as a complete solution for established chronic back pain. Set realistic expectations: aim for significant pain reduction and improved function rather than complete pain elimination.
For comprehensive guidance on safe practices, review how to use an inversion table safely as part of your multi-modal approach to back pain management.
What Are Common Mistakes When Using Weight Loss for Back Pain?
People make several critical mistakes when attempting to lose weight for back pain relief. These errors can delay results, worsen pain, or lead to unsustainable outcomes that result in weight regain.
Critical mistakes to avoid:
Mistake 1: Excessive calorie restriction
Crash diets or very low-calorie approaches cause muscle loss, including core muscles that support your spine. This weakens spinal stability and can actually increase back pain despite weight loss. Aim for moderate deficits of 500-750 calories daily rather than extreme restriction.
Mistake 2: High-impact exercise while in pain
Starting intense exercise programs like running or CrossFit while experiencing significant back pain often leads to injury and setbacks. Choose low-impact activities initially, progressing gradually as pain decreases and fitness improves.
Mistake 3: Ignoring nutrition quality
Focusing solely on calories while eating inflammatory foods limits pain relief potential. A 1,500-calorie diet of processed foods produces different outcomes than 1,500 calories of whole, anti-inflammatory foods. Prioritize food quality alongside quantity.
Mistake 4: Neglecting core strengthening
Weight loss without core muscle development leaves your spine vulnerable. As you lose weight, actively build the muscular support system that will protect your back long-term. Start with gentle exercises and progress systematically.
Mistake 5: Expecting immediate results
Becoming discouraged when pain doesn’t improve within 2-3 weeks leads many people to abandon their efforts. Remember that clinically significant improvements typically appear around 8-14 weeks. Maintain consistency through the initial period.
Mistake 6: Using pain as the only metric
Relying exclusively on pain levels to measure progress misses other important improvements. Track multiple indicators including weight, measurements, activity tolerance, sleep quality, and mood. These often improve before pain decreases significantly.
Mistake 7: Attempting weight loss during acute injury
Starting a weight loss program during an acute back injury or flare-up divides your body’s resources between healing and adaptation. Address acute pain first, then implement weight loss strategies during recovery phases.
Mistake 8: Skipping professional guidance
Self-directed weight loss without medical clearance can be dangerous for people with certain conditions. Consult healthcare providers before starting, especially if you have diabetes, heart disease, or other chronic conditions alongside back pain.
Learn about who should not use an inversion table to ensure any complementary therapies you consider are safe for your specific situation.
Frequently Asked Questions
How quickly will I notice back pain improvement after losing weight?
Most people notice initial improvements within 8-14 weeks of consistent weight loss efforts, typically after losing 5% of their body weight. Some experience relief sooner, while others with chronic pain or structural damage may require more time and greater weight loss.
Does belly fat specifically cause more back pain than other fat?
Yes, abdominal fat causes disproportionate back pain because it shifts your center of gravity forward, forcing your spine into compensatory positions. Visceral fat around organs also produces more inflammatory molecules than subcutaneous fat, increasing pain through biological mechanisms.
Can I lose weight safely while dealing with severe back pain?
Yes, but choose activities that don’t aggravate your pain. Focus on dietary changes for calorie reduction and gentle activities like walking in water, seated exercises, or recumbent cycling. Consult a physical therapist for safe exercise modifications specific to your condition.
Will weight loss help sciatica pain specifically?
Weight loss often helps sciatica by reducing pressure on nerve roots and decreasing inflammation around compressed nerves. However, sciatica caused by structural issues like herniated discs may require additional treatments beyond weight loss for complete relief.
How much weight do I need to lose to see any difference in back pain?
The threshold for clinically meaningful improvement is approximately 5% of your total body weight. For a 200-pound person, this equals 10 pounds. Greater weight loss typically produces proportionally better results, with 10-15% loss showing substantial improvements.
Does the speed of weight loss affect back pain relief?
Gradual weight loss of 1-2 pounds weekly produces better outcomes than rapid weight loss. Slow, steady loss preserves muscle mass, allows tissues to adapt, and creates sustainable habits. Rapid weight loss often causes muscle loss that can worsen back pain.
Can weight loss reverse disc degeneration or arthritis?
Weight loss cannot reverse existing structural damage but can slow progression and significantly reduce symptoms. Decreased load allows remaining healthy tissue to function better, inflammation to decrease, and pain to improve despite persistent structural changes.
Should I wait until I lose weight before starting inversion therapy?
No, you can safely use inversion therapy while losing weight if you’re within the weight capacity of your equipment. Most quality inversion tables accommodate 250-300 pounds. Check inversion table buying guides for weight capacity specifications.
Will I need surgery if weight loss doesn’t eliminate my back pain?
Not necessarily. Many people achieve satisfactory pain management through conservative treatments even when pain persists. Surgery becomes necessary only when conservative approaches fail and you have progressive neurological symptoms or severely impaired function.
Does weight loss help back pain in older adults as much as younger people?
Weight loss benefits older adults, though results may develop more slowly due to reduced healing capacity and longer pain duration. Older adults should emphasize muscle preservation through adequate protein intake and resistance training alongside weight loss.
Can I use weight loss supplements safely while dealing with back pain?
Most weight loss supplements lack strong evidence and may interact with pain medications. Focus on proven strategies: calorie reduction, whole foods, and appropriate activity. Consult your healthcare provider before using any supplements, especially if taking medications.
How do I maintain weight loss and back pain relief long-term?
Sustainable maintenance requires permanent lifestyle changes rather than temporary diets. Establish habits you can maintain indefinitely: balanced nutrition, regular activity, stress management, and adequate sleep. These same habits support both healthy weight and spinal health.
Conclusion
Weight loss provides substantial back pain relief through multiple mechanisms: reducing mechanical load, decreasing inflammation, improving posture, and enhancing mobility. Research consistently demonstrates that losing just 5% of body weight produces clinically significant improvements for most people with chronic back pain.
The evidence is clear: every pound lost removes up to four pounds of pressure from your lower back, allowing discs to recover, joints to heal, and pain to subside. Studies show that 50% of people who lose more than 5% of their body weight achieve meaningful pain reduction, while 73% experience improved disability scores.
However, weight loss works best as part of a comprehensive approach. Combine gradual, sustainable weight loss with core strengthening, appropriate physical activity, and complementary therapies like lumbar pain relief techniques for optimal results.
Take action today:
Set realistic goals: Aim for 5-10% weight loss over 3-6 months as your initial target
Focus on nutrition quality: Emphasize anti-inflammatory whole foods alongside calorie reduction
Start appropriate activity: Choose low-impact exercises that don’t aggravate your current pain level
Track multiple metrics: Monitor weight, pain levels, activity tolerance, and quality of life indicators
Seek professional guidance: Work with healthcare providers to create a safe, effective plan for your specific situation
Consider complementary approaches: Explore inversion therapy and other evidence-based treatments alongside weight loss
Maintain consistency: Remember that meaningful improvements typically appear around 8-14 weeks; persist through the initial period
Weight loss offers a powerful, evidence-based tool for back pain management that addresses root causes rather than merely masking symptoms. By reducing the load your spine carries and decreasing systemic inflammation, you create conditions that allow your body to heal naturally. Combined with other proven strategies, weight loss can transform your relationship with back pain and restore the active, pain-free life you deserve.
SEO Meta Title: Does Losing Weight Help Back Pain? 2026 Evidence-Based Guide
Meta Description: Discover how weight loss reduces back pain through proven mechanisms. Learn the 5% threshold, timeline for relief, and best methods backed by research.
Tags: weight loss, back pain relief, spine health, lumbar pain relief, back pain treatment, sciatica treatment, inversion therapy, spinal decompression, core strengthening, chronic pain management, BMI and back pain, anti-inflammatory diet